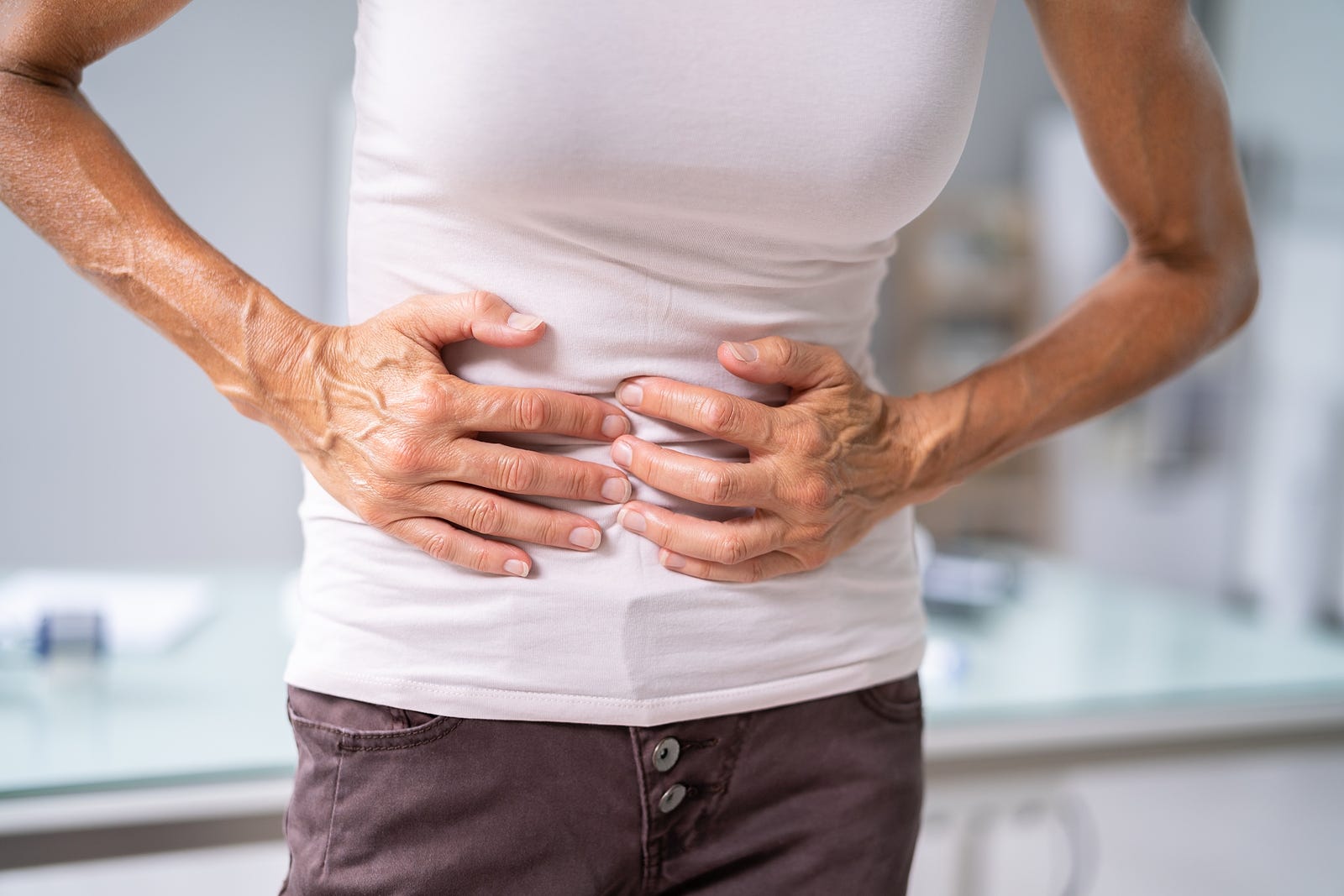
- Diverticulitis is an inflammation or infection of small pouches called diverticula that can develop along the walls of your intestines
- Diverticulitis can cause abdominal pain, constipation, diarrhea, nausea, vomiting, fever and rectal bleeding
- More severe cases can lead to serious complications, including abscesses, fistulas and intestinal blockage
- Restoring your gut microflora and cellular energy production are key to resolving diverticulitis
- Eating foods that support Akkermansia, such as polyphenol-rich fruit, and other beneficial bacteria, and avoiding linoleic acid, are important for diverticulitis; rectal CO2 insufflation may also help
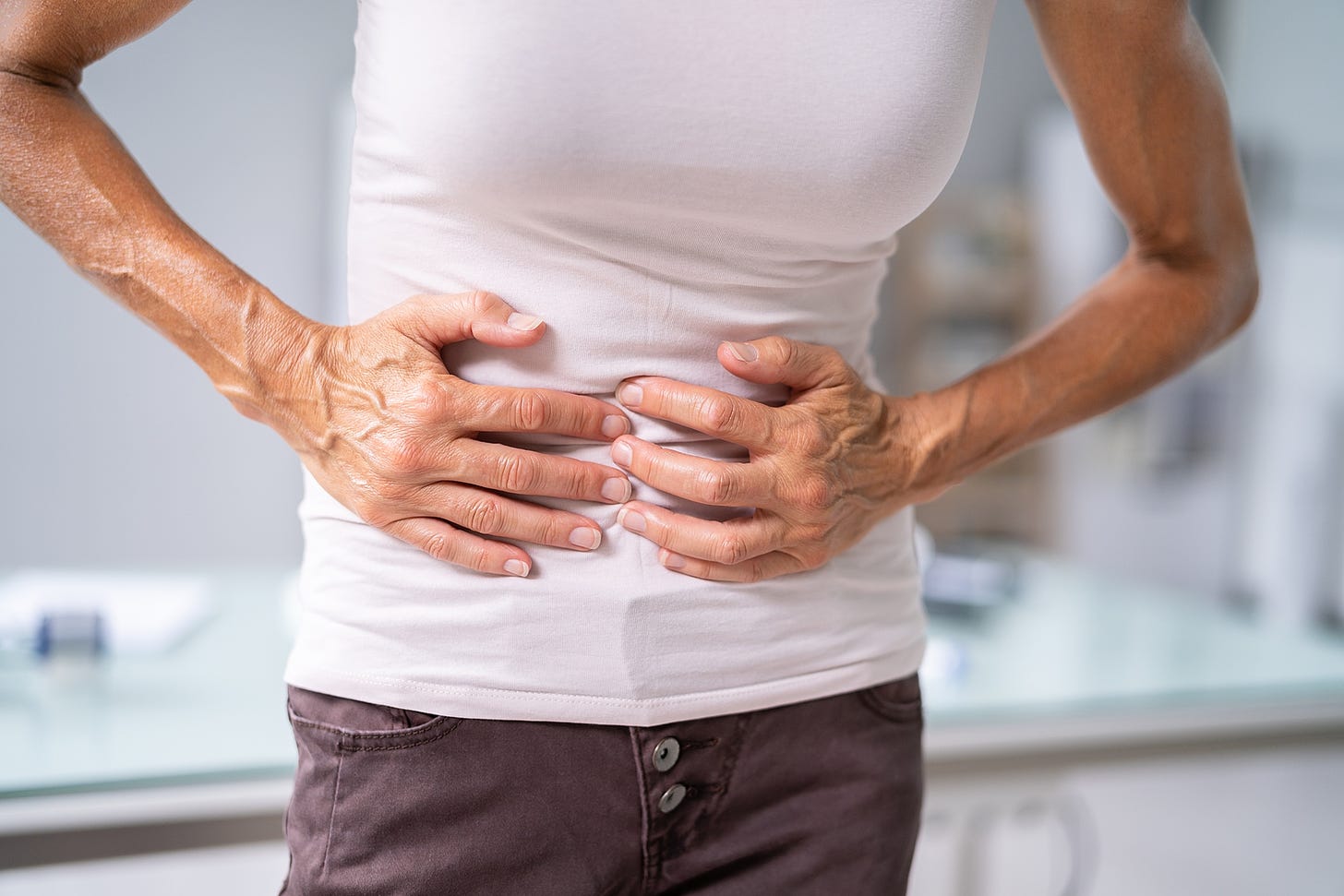
Diverticulitis is an inflammation or infection of small pouches called diverticula that can develop along the walls of your intestines. The formation of these pouches is known as diverticulosis, a common condition that typically causes few or no symptoms. However, when these pouches become inflamed or infected, it leads to diverticulitis, which can be painful and may lead to serious complications.
Diverticulosis is common in the U.S. and other parts of the world where heavily processed diets are the norm. It’s estimated that 30% of Americans over 50 have diverticulosis, which rises to 50% of those over 60% and 75% in people over 80.1
Most often, the condition affects the sigmoid colon, a section of the large intestine near the end of the digestive tract. Among those with diverticulosis, about 4% develop diverticulitis.2
What Are the Symptoms of Diverticulitis?
You can have diverticulosis and not know it, since it often causes no symptoms. But in the case of diverticulitis, it’s typically a different story. Common symptoms include:3
•Abdominal pain — When diverticula become inflamed, they cause the surrounding tissues in the intestinal wall to also become inflamed. This inflammation can lead to pain that’s typically felt in the lower left side of the abdomen and may be severe.
The pain may also spread to your pelvis and back. In people of Asian descent, diverticulosis may occur more often in the first part of the colon, so diverticulitis in that region may cause pain in the upper right abdomen.4
•Bowel changes — The inflammation associated with diverticulitis can affect the movement of the bowel, leading to disruptions in the normal rhythm of digestion. This can result in constipation or diarrhea, along with bloating and gas. Feelings of fullness can also occur.
•Nausea and vomiting — Gastrointestinal irritation may lead to nausea while increased movement of the intestines in an attempt to expel irritants and bacteria may lead to vomiting. In more severe cases, the inflammation can lead to a partial or complete blockage of the intestine, which can trigger vomiting.
•Fever — When diverticula become inflamed, they can also become infected, usually by bacteria. The fever is a sign that your body is actively fighting an infection.
•Rectal bleeding — As diverticulitis progresses, the inflamed diverticula can cause small blood vessels to stretch and rupture, leading to bleeding. This can result in blood appearing in the stool.
Diverticulitis can be classified as acute, which occurs suddenly and often causes intense abdominal pain, fever and nausea, or chronic, with persistent symptoms due to the ongoing inflammation.
More severe cases can lead to serious complications, which are sometimes the first sign of the disease. Each year, about 200,000 people are hospitalized due to diverticulitis, while 71,000 are hospitalized with diverticular bleeding.5 Complications may include:6
- Abscesses
- Perforation, or a hole, in your colon
- Fistulas, an abnormal tunnel between your colon and another area of the body, such as your bladder
- Intestinal blockages
- Peritonitis, an infection of the abdominal cavity
What Causes Diverticulitis?
Certain genes may increase your risk of diverticulitis, but lifestyle factors also play a role, including:7
- Eating ultra-processed foods
- Inactivity
- Using certain medications, including nonsteroidal anti-inflammatory drugs (NSAIDs) and steroids
- Obesity
- Smoking
While a number of factors contribute to diverticulitis, a disrupted microbiome and eating a highly processed, low-fiber diet are chief among them. Dietary fiber is crucial for maintaining a healthy digestive system. It helps to bulk up your stool and softens it, making it easier to pass through the colon. This reduces the strain and pressure in your colon during bowel movements.
When your diet lacks sufficient fiber, your stools become harder and smaller, requiring your colon to exert more pressure to move them along. This increased pressure can cause your colon’s muscular wall to develop weak spots.
Over time, the continuous pressure may force the inner lining of your colon through these weak spots in the muscle layer, forming diverticula. Further, a diet low in fiber keeps the intra-colonic pressure elevated because of the harder, smaller stools and the greater effort needed to expel them.
This sustained high pressure is believed to not only contribute to the formation of diverticula but also increase the risk of these diverticula becoming inflamed or infected, leading to diverticulitis. As noted in Cureus:8
“Many theories have been suggested for the different etiologies of diverticular disease, and the most common cause is believed to be a low-fiber diet. It is believed that diets low in fibers are associated with increased intra-colonic pressure, which leads to diverticula formation.”
Diverticulitis Linked to Gut Microbiome Composition
Researchers with Massachusetts General Hospital and Harvard Medical School collected stool samples from 121 women with severe diverticulitis and compared them to stool samples from 121 women without the condition.9 They conducted a detailed analysis of the overall microbial community structures and metabolomic profiles in the collected samples, revealing significant differences between the groups.
Women with diverticulitis had more pro-inflammatory agents such as the microbe Ruminococcus gnavus, 1,7-dimethyluric acid and various histidine-related metabolites. There was also a notable depletion of butyrate-producing bacteria, which are known for their anti-inflammatory properties, as well as a reduction in anti-inflammatory ceramides.
The study highlighted how microbial composition may influence the protective association between a fiber-rich diet and diverticulitis, suggesting that dietary fiber’s protective effects can be significantly altered by a person’s existing gut microbiota composition. A review published in the Journal of Personalized Medicine further described gut microbiota’s potential role in diverticulitis, noting:10
“Changes in microbiota composition have been observed in patients who were developing acute diverticulitis, with a reduction of taxa with anti-inflammatory activity, such as Clostridium cluster IV, Lactobacilli and Bacteroides.
Recent observations supported that a dysbiosis characterized by decreased presence of anti-inflammatory bacterial species might be linked to mucosal inflammation, and a vicious cycle results from a mucosal inflammation driving dysbiosis at the same time.
An alteration in gut microbiota can lead to an altered activation of nerve fibers, and subsequent neuronal and muscular dysfunction, thus favoring abdominal symptoms’ development.”
Restoring Your Gut Microflora and Cellular Energy Production Are Key
Dysbiosis, or an imbalance of microbial communities, in your gut plays a central role in the development of diverticulitis.11 A balanced gut microbiota helps reduce inflammation in the colon. Certain beneficial bacteria produce short-chain fatty acids (SCFAs) like butyrate, which have anti-inflammatory properties. These SCFAs help maintain the health of the colon lining and prevent inflammation that can lead to diverticulitis.
A robust intestinal barrier can also prevent bacterial fragments from entering your bloodstream, whereas a compromised barrier allows these harmful fragments through while blocking SCFAs. However, most people have dysfunctional mitochondria, and if you don’t have enough mitochondria, you can’t create cellular energy efficiently enough to ensure a healthy gastrointestinal tract.
Your gut contains primarily two types of gram-negative bacteria: beneficial and pathogenic. The beneficial ones include obligate anaerobes, which cannot survive in the presence of oxygen and are essential for health. They do not produce harmful endotoxins and contribute positively by producing SCFAs like butyrate, propionate and glucagon-like peptide-1 (GLP-1).
Proper gut function requires energy to maintain an oxygen-free environment in the large intestine, where 99% of gut microbes reside. Insufficient energy leads to oxygen leakage, which harms obligate anaerobes while not impacting the facultative anaerobes, thereby disrupting the balance of the microbiome.
Pathogenic bacteria, or facultative anaerobes, can survive in oxygen and are harmful, as they possess endotoxins in their cell walls. In short, enhancing mitochondrial energy production is crucial for maintaining a healthy gut environment. When you do that, it helps suppress the growth of pathogenic bacteria and support beneficial microbial populations, which in turns reduces your risk of diverticulitis.
Widespread use of antibiotics can also disrupt the microbiome by killing both beneficial and harmful bacteria, leading to a dominance of pathogenic bacteria which produce harmful endotoxins. Optimizing your mitochondrial function is, however, one of the most important strategies you can do to optimize your cellular energy, so it’s at the core of almost everything that you do to improve your health.
How to Restructure Your Microbiome
Akkermansia, highly beneficial bacteria in your large intestine, plays a crucial role in maintaining gut health and should constitute about 10% of the gut microbiome. However, it is absent in many individuals, likely due to inadequate mitochondrial function and resultant oxygen leakage in the gut.
Eating foods that support Akkermansia, such as polyphenol-rich fruit, and other beneficial bacteria, and avoiding foods like linoleic acid — found in vegetable and seed oils in most processed foods — that destroy these bacteria, will help to restructure your microbiome in a positive way. You can also use an Akkermansia probiotic supplement.
One of the reasons Akkermansia is so important is because it produces mucin, a thick, protective gel-like substance that lines various parts of the body, including the gastrointestinal tract. Mucin forms a protective barrier on the gut lining, shielding the epithelial cells of the intestinal wall from mechanical damage, chemical irritation from stomach acids and digestive enzymes, and pathogenic organisms like bacteria and viruses.
Mucin also supports the immune system by trapping potential pathogens and other foreign particles, which are then expelled from the body through the digestive process. It also contains antibodies and antimicrobial peptides that help fight off infections.
Lastly, mucin serves as a food source for other beneficial gut bacteria. This relationship is essential for digestive health, as the bacteria fed by Akkermansia aid in digestion, produce essential nutrients, and help maintain an overall balance of gut flora.
Increasing CO2 Likely Beneficial
Carbon dioxide (CO2) is a driver of energy production, as it improves the delivery of oxygen into your cells. While CO2 is typically thought of as nothing more than a harmful waste product of respiration, and a “pollutant” that endangers the planet, the reality is that it’s essential for most life on Earth. In fact, CO2 appears to be a more fundamental component of living matter than oxygen.12
“Really, every condition you can think of, both physiological and mental, can be remediated, and in many cases cured, by increasing endogenous CO2 production and decreasing degradation,” Georgi Dinkov says.
Importantly, CO2 allows for more efficient energy production in your mitochondria, which is why people who live or spend time at higher altitudes tend to be healthier and have fewer chronic health problems such as asthma. The reason for this is because the pressure of CO2 relative to oxygen is greater at higher altitudes.
In order to have sufficient CO2 production, you need healthy mitochondria, because CO2 is produced exclusively in the Krebs cycle in the mitochondria. If you have mitochondrial dysfunction, if you’re hypothyroid or have high levels of inflammation, as is the case in diverticulitis, then you will not be producing enough CO2.
While it’s important to optimize your endogenous (internal) production of CO2, exogenous delivery or supplementation will produce the greatest benefits, as you can deliver far greater amounts than your body can produce. Such strategies include:
- Breathing into a paper bag
- Drinking carbonated water and other carbonated beverages
- CO2 baths
- A special suit into which CO2 is pumped
- Taking small amounts of baking soda in your drinking water
A book written in 1905 by Achilles Rose, M.D. discusses delivery by rectal insufflation. During rectal CO2 insufflation, a small tube or catheter is inserted into the rectum, and a controlled amount of CO2 is gently infused. This is a highly effective way to deliver CO2.
I am currently in the process of setting up an IRB (Institutional Review Board) approved study that will be exploring the therapeutic value of administering CO2 gas rectally to reverse the damage caused by decades of excess LA consumption that caused a radical decrease in mitochondrial function and cellular energy production resulting in a compromised oxygen gradient differential in the large intestine that allows pathogenic bacteria to become squatters and occupy the spaces of the obligate anaerobic species like Akkermansia that provide benefits and do not produce toxic endotoxin.
ORIGINALLY PUBLISHED BY: DR. JOSEPH MERCOLA.
Sources and References
- 1, 3, 4 Cleveland Clinic, Diverticulosis
- 2 Cleveland Clinic, Diverticulitis
- 5, 6 National Institute of Diabetes and Digestive and Kidney Diseases, Definition & Facts for Diverticular Disease
- 7 National Institute of Diabetes and Digestive and Kidney Diseases, Symptoms & Causes of Diverticular Disease
- 8 Cureus. 2023 Aug; 15(8): e43158
- 9 Nat Commun. 2024 Apr 29;15(1):3612. doi: 10.1038/s41467-024-47859-4
- 10 J Pers Med. 2021 Apr; 11(4): 298
- 11 Neurogastroenterology & Motility May 27, 2023
- 12 Conscious Breathing Carbon Dioxide, Physiology